In cases where aches and pains are rooted in a problem with the patient’s musculoskeletal system, the physician may order a diagnostic imaging test to determine the cause. There are multiple types of diagnostic imaging techniques at a physician’s disposal, such as ultrasound, computed tomography (CT) scans, magnetic resonance imaging (MRI), and x-rays. Depending on the needs of the clinician, ultrasound may provide some advantages over its sister techniques for musculoskeletal conditions. “Some common reasons we do musculoskeletal ultrasound are to evaluate the rotator cuff in the shoulder, to look for Achilles tendon tears and to evaluate elbow tendon problems,” said diagnostic radiologist Michael C. Forney, M.D., from the Cleveland Clinic. “But an ultrasound can be performed on most joints as long as the area evaluated is limited to just part of the joint.”
When is ultrasound used instead of MRI?
It is important to note that ultrasound and MRI look at the body in different ways and can provide physicians with unique insights. MRI uses powerful magnets to produce 3-D anatomic images and is a high-contrast resolution modality that can determine changes in the quality of tissue. For example, in the case of a muscle injury, MRI images will often show a bright signal that reveals there is more water in the muscle, which is a sign of injury. On the other hand, ultrasound uses high-frequency sound waves to examine organs and structures. This diagnostic imaging technique is a high-spatial resolution modality that produces detailed images of structures, particularly those near the skin's surface.
Ultrasound advantages
One of the significant advantages of ultrasound as a diagnostic imaging technique is that it does not use radiation like MRI and CT do. In addition to the lack of radiation, it can show diagnostic images in real-time. Thus, it has the unique ability to reveal abnormalities that can only be viewed with motion, such as impingent of the bursa in the shoulder. In addition, patients do not have to enter the bore or tube of a scanner as they do with MRI or CT. Ultrasound has the ability to show diagnostic images with better resolution and detail than MRI. For example, the tendons in the fingers are usually seen with a higher level of detail via an ultrasound scan than with MRI. Moreover, ultrasound can be used for other applications, such as guided injections. For example, when performing a corticosteroid shot into a joint, the clinician can use the ultrasound to view the structure and ensure the injection is hitting the correct location. In these cases, the transducer may be protected with an ultrasound cover to prevent cross-contamination and the transmission of healthcare-acquired infections. In addition, the physician may employ the use of a needle guide to ensure greater precision and accuracy while performing the injection. Image-guided joint injections can also be performed with CT scans or x-rays; however, ultrasound does not use radiation and there is no need to inject a contrast dye. Therefore, some physicians may opt for an ultrasound-guided procedure because of its ease of use and increased patient comfort.
What to expect during an ultrasound scan
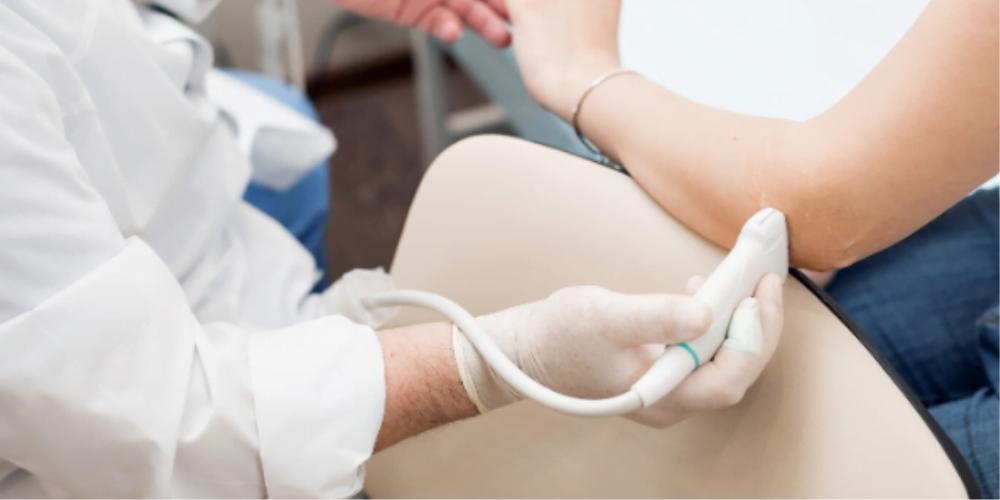
Ultrasound scans are typically performed by a specially trained technician or sonographer. The clinician will move the handheld probe over the target area. Afterwards, the diagnostic images from the ultrasound will be taken to a radiologist who will then interpret them, usually within 24 hours.
When an MRI is necessary
Like any diagnostic imaging technique, ultrasound has its limitations and there are situations which call for an MRI. When physicians need to evaluate damage to bone, cartilage, or other structures inside and around the joint, MRI is the more adequate choice. Medical practitioners also prefer MRI when evaluating conditions that impact deep or large areas, because ultrasound is only able to examine a small area per scan.