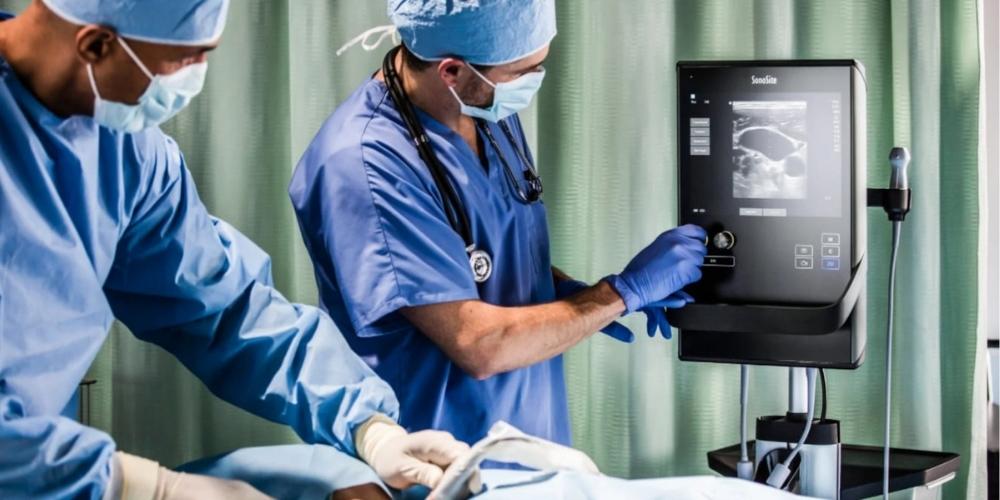
Ultrasound guidance has become a common technique for many practitioners outside the radiology department, thanks to technological advancements in point-of-care ultrasound (POCUS). In the last ten years, ultrasound machines have been introduced in smaller, more portable variations with improved image quality. This has allowed them to make their way into other departments outside radiology.
What exactly is POCUS?
Point-of-care ultrasound is a very useful imaging technique, notably for medical staff working in emergency medicine. Vastly used in Europe, it is now part of emergency medicine training in the US and Canada. The practitioner performs all acquisition and interpretation of images at the point of care and uses this information immediately to address specific issues to guide therapy in progress. Note that bedside ultrasound is like a subset point of care ultrasound (POCUS). POCUS is a broad term to designate the many scenarios (ER, ambulance, helicopter, at the bedside, etc.) in which portable ultrasound can be used.
In what ways can POCUS benefit quality of care?
POCUS can benefit a lot of different specialties, but it shines best when used in the diagnostic process of critically ill patients in emergency medicine. Combined with a physical assessment, many clinicians agree that POC ultrasound works well to efficiently reach a reliable diagnosis. This is undoubtedly helpful in determining the next steps in the patient’s treatment.
In the emergency department, life of patients can also depend on the time necessary to formulate a diagnosis. A study published in 2017 demonstrated that while POCUS did not help achieve a different diagnosis, the average time needed to formulate it was significantly lower in diagnosing dyspnea. All these benefits lead to an improved patient safety, demonstrating how POCUS can be valuable in an emergency setting.
Over the years, protocols have been established to facilitate clinical decisions with the help of POCUS, covering every emergency specialty. They require proper training to meet their clinical needs. Here is a small list of 6 intensively used protocols:
eFAST
Trauma ultrasound protocol to detect free fluids. It can also quickly detect a pneumothorax.
BLUE
Used when the patient suffers from acute respiratory distress. Detects most lung disorders without a CT scan.
RADiUS
Rapidly assess dyspnea in patients with unexplained acute respiratory or chest complaints.
RUSH
Determine underlying etiology of hypotension, by examining the heart (pump, tank, and pipes).
FEEL
Echocardiography in emergency life support for cardiac arrest.
ACES
Quickly establish a diagnosis for hypotension in 6 windows: cardiac, peritoneal, pleural, IVC, and aortic views.
Some organizations around the world have started to recommend the use of POCUS for various procedures. For example, the Society of Hospital Medicine advocates its use for central and peripheral vascular access, provided that users are properly trained to avoid complications including the transmission of HAIs. In the UK, the National Institute for Health and Care Excellence who provides national guidance and advice to improve health and social care, mandated the use of ultrasound guidance for CVC. They were followed by a National Patient Safety Agency report requiring it for pleural procedures. Ultrasound guided procedures like those are executed with more ease, without the need for a radiology room. They increase patient safety by using non-invasive guidance, without requiring a radiology room.
Ultimately, POCUS can be very useful for patients that are not easily moveable. In the case of ER, we already discussed POCUS use on critically ill patients, but we can also add patients in quarantine, especially in this pandemic era. In emergency departments around the world, practitioners had to adapt to answer the exponential demand they were facing. Lung ultrasound is comparable to chest radiography in the diagnosis of coronavirus and the assessment of its severity. Additionally, it brings along a myriad of advantages: no radiation exposure, no patient transport to the imaging suite (thanks to POCUS), and a high speed of execution. Quarantined patients can be examined with POCUS at their bed, eliminating the need of an imaging suite for them.
It is also important for practitioners to be aware of the risks. POCUS can be a great ally for quarantined patients since they no longer need to break isolation to be examined. However, the machine must follow a rigorous disinfection protocol to make sure it won’t become the source of cross-contamination. The whole machine should be disinfected following The CDC’s recommendations after every patient. Probes that come in contact with non-intact skin should also be covered with a single-use probe cover.
POCUS is an ultrasound technique that helped ultrasound find its way to many different specialties. It has become so useful that it will soon be sent into space to assist astronauts in their research on the heart. Ultimately, it also has the potential to help decrease healthcare disparities. A simple system called the Butterfly POCUS can turn smartphones into echo systems. This could be coupled with AI, and enable novice ultrasound technicians or physicians to acquire the images and interpret the exam, supporting rural clinicians, for example.