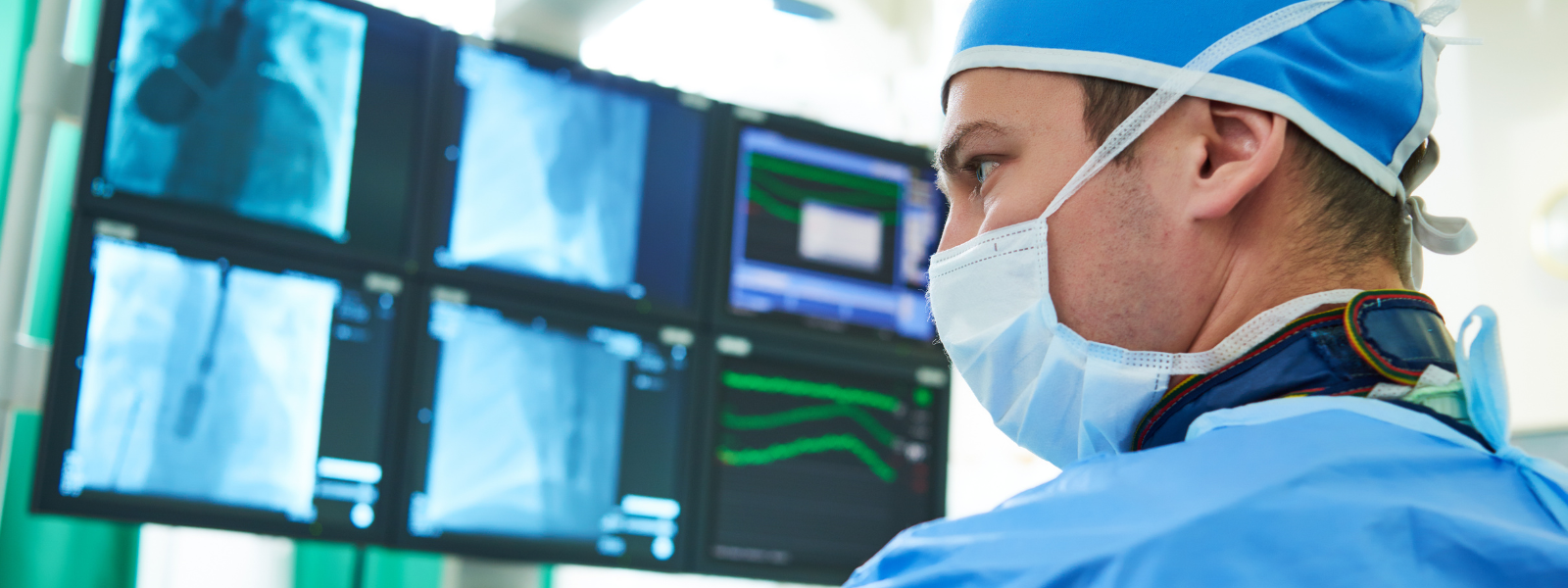
In the demanding field of interventional radiology (IR), professionals are frequently exposed to the risk of work-related musculoskeletal disorders (WRMSDs), a health concern that's gaining increasing attention in today's medical world. The intricate and physically taxing nature of their work, often involving long hours in lead shielding for radiation protection, makes them prone to such conditions. In this article, we’ll discuss everything you need to know for Injury-Proofing Your Work - Ergonomics in Interventional Radiology.
Interventional radiology provides a less intrusive alternative to open surgery, offering treatments like stent placement, embolization, and image-guided device insertion. These methods are extensively used in treating brain, heart, and gastrointestinal diseases.
IR therapies utilize imaging modalities for precise and safe procedures. Despite the rapid advancement of IR devices, ergonomic considerations for practitioners have been largely overlooked, apart from radiation health management.
According to an article published in Procedia Manufacturing in 2015, interventional radiologists often work under challenging conditions. They wear heavy radiation protective gear, operate in poorly lit environments causing eyestrain, and adopt uncomfortable postures due to the inflexibility of equipment setup.
All these factors contribute to fatigue, increase the risk of mishaps, and can lead to musculoskeletal issues. Physicians also manipulate small devices while wearing sterilized gloves which can cause neuromuscular fatigue and potentially affect the movement of catheters.
Furthermore, the industry lacks standard ergonomic design guidelines and training to minimize such risks, and the manuals provided are often difficult to understand. These issues not only deter the use of interventional radiology devices but also elevate the risk of malpractice.
Authors of an article published in the Journal of Vascular and Interventional Radiology in 2021 remarked that research into ergonomics within interventional radiology is still in its early stages and added that female operators seem to be more susceptible to suffering from musculoskeletal issues.

How Work-Related Musculoskeletal Disorders are Affecting Female and Male Practitioners
A study published in Cureus in 2021 about the prevalence and risk factors of work-related musculoskeletal disorders among healthcare professionals, with a particular focus on gender differences, suggests that female representation in studies related to the topic is relatively low, averaging 25.7%.
Interestingly, 72% of female practitioners reported WRMSDs, compared to 46.6% of men. Women also seemed to experience more upper extremity pain, while men reported more lumbar pain. Factors contributing to these discrepancies could include the size and design of procedural tools.
In terms of specific professions, interventional cardiologists showed a significant increase in cervical pain due to the use of fluoroscopic monitors. Endoscopists reported a high prevalence of musculoskeletal injury, with the most common areas of pain being the neck, lower back, and hand. Among orthopedic surgeons, frequent back pain was reported, often associated with wearing ill-fitting lead aprons.
Self-reported physical discomfort among all respondents averaged at 72.4%, with WRMSDs most commonly found in the lumbar spine, cervical spine, shoulder, and hands.

In the same article, the authors also noted that interventional cardiologists have seen a significant rise in cervical pain, largely due to the use of fluoroscopic monitors. When compared to non-interventional cardiologists, electrophysiologists showed a higher prevalence of both cervical and lumbar spondylosis.
Additionally, a large proportion of endoscopists reported musculoskeletal injuries, with many attributing the pain to specific procedures like endoscopic retrograde cholangiopancreatography (ERCP). Common areas of discomfort included the neck, lower back, and hands, with de Quervain’s tenosynovitis and cervical radiculopathy being common injuries. Additionally, ill-fitting lead aprons were reported by a majority of orthopedic surgeons, contributing to increased back pain.
Key insights:
- Prevalence of cervical spondylosis among electrophysiologists: 20.7%
- Prevalence of cervical spondylosis among non-interventional cardiologists: 5.5%
- Prevalence of lumbar spondylosis among electrophysiologists: 25.9%
- Prevalence of lumbar spondylosis among non-interventional cardiologists: 16.7%
- Percentage of endoscopists reporting musculoskeletal injuries: 48-67%
- Percentage of endoscopists attributing pain to ERCP: 32-74%
- Common areas of pain: neck (24-46%), lower back (17-57%), and hand (33%)
- Common injuries: de Quervain’s tenosynovitis (16%), cervical radiculopathy (12%)
- Orthopedic surgeons reporting ill-fitting lead aprons: 74.2%
- Orthopedic surgeons stating the lead was too large: 83.9%
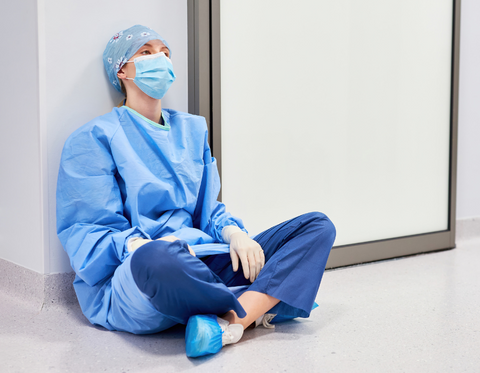
Burnout in Interventional Radiologists
Work-related musculoskeletal disorders can also contribute to a stress syndrome known as burnout, characterized by emotional exhaustion, physical fatigue, and cognitive weariness. Burnout can have detrimental physical and psychological effects, potentially leading to changes in perception of pain, fatigue, cardiovascular issues, and depression.
According to a study presented in an article published in Medicina in 2021, surgeons that were experiencing physical discomfort reported significantly less job satisfaction, higher levels of burnout, and an increased tendency toward callousness compared to their counterparts not fearing career longevity loss. This could potentially discourage younger individuals from pursuing careers in interventional radiology, particularly if they are aware of the risks associated with WRMSDs.
Therefore, there is a need for further research into risk factors within interventional radiology, assessment of their impact on productivity, patient care, and satisfaction, and identification of interventions to promote the wellbeing of these professionals.
Ergonomic Considerations Depending on the Procedure
In the article Ergonomics in Interventional Radiology: Awareness Is Mandatory, the authors proposed a comprehensive guide of ergonomic practices per procedure that interventional radiologists can execute to prevent work-related musculoskeletal disorders.
Ultrasound-Guided Procedures
Performing ultrasound-guided procedures often requires maintaining awkward positions of the trunk, neck, and upper extremities. Combined with sustained or forceful gripping and downward force exerted with the transducer, these factors increase discomfort and injury risk.
WRMSDs in the hand and wrist have been observed to be associated with performing over 100 scans per month, average scan times exceeding 25 minutes, posture, high-pressure handgrip, and shorter stature (less than 63 inches). Posture, axial twisting, and excessive reach during exams can also contribute to back, neck, and shoulder pain.
To mitigate these risks, interventional radiologists should diversify their exam postures throughout the day. Implementing hand stretching exercises can help alleviate muscle tension. To reduce strain on the dominant hand, alternating the hand that holds the transducer is recommended. Maintaining neutral body positioning and limiting arm abduction can be facilitated by placing the monitor directly in front of the operator. Finally, using indirect lighting can help prevent visual fatigue.
Angiography and Cone-Beam Computed Tomography Procedures
Interventional radiologists working in the angio suite should adhere to guidelines that help limit radiation exposure. One key protective item is the lead apron, which can weigh up to 15 pounds. However, this heavy piece of equipment can put pressure on the lumbar or cervical discs.
While further investigations are required to understand the impact of these protective devices on WRMSDs, current recommendations suggest the use of a two-part coat or one with a suitable belt to evenly distribute the weight across the shoulders and waist.
Protective aprons have evolved to be lighter and may consist of composite or fully lead-free materials. Although these aprons reduce spinal pressure, they do not eliminate additional pressure load, hence the need to remove the coat between procedures.
There are devices designed to entirely replace the apron, such as freestanding, suspended, or movable shields. However, care must be taken to avoid uncomfortable positions due to space limitations while using them. Large lens leaded glasses with side shields are also recommended, but their adoption is limited due to discomfort and weight issues.
Attention should be given to the position of the cervical spine, which is often extended and rotated in the angio suite because of device and monitor placements. Ideally, ergonomic medical displays should be used and the screen should be situated in front of the operator, just below eye level, at a downward viewing angle of 10°–15° to reduce neck strain. Ceiling-mounted monitors are advantageous as they can be positioned flexibly. A large screen and a broadcast video system can enable ergonomic multimodal visualization, reducing fatigue and further decreasing radiation exposure.
Other important considerations in the angio suite include adjusting the table height to maintain the elbow joint in a neutral position most of the time, thereby preventing the operator from bending forward. Standing on softer surfaces such as mats or insoles can also provide more comfort and less fatigue than standing on hard floors for long periods.
CT and PET Scan Procedures
Despite the radiation exposure concerns, which are identical to those in the angio suite, the design of these systems necessitates the operator to work closely to or inside the CT tunnel, often resulting in uncomfortable or poor postures. Consequently, operators may find themselves frequently leaning or bending during procedures.
The use of surgical nippers, advanced visualization techniques, fusion imaging, and electromagnetic navigation could potentially decrease procedural time and enhance the position of interventional radiologists.

MRI-Guided Interventions
Open field magnets, as compared to CT scans, can enhance the procedure by offering extensive access to the bore, thereby improving the position of interventional radiologists. However, operating under powerful magnetic fields comes with specific prerequisites. Safety considerations encompass the biological impacts of magnetic fields, potential burns and hearing damage, projectile effects, and the compatibility of additional equipment.
Noise is a significant concern in this setting, potentially impacting focus and productivity. Hence, the selection of suitable materials for operator protection, such as noise-cancelling headphones, and the use of noise-controlling elements in the ceiling, floor, and walls are imperative. Regular upkeep of the equipment is also advised.
Recommendations Outside the Work Environment
Physical Exercise as a Preventive Measure
Maintaining flexibility in the spine and strength in the back muscles can help to resist fatigue. Also, avoid prolonged periods in lordotic (exaggerated spinal curve) or fully flexed positions, as well as sudden and awkward bending movements, particularly early in the day.
When lifting objects, do it slowly with a balanced, slightly bent spine and relaxed muscles, keeping the weight close to and in front of your body.
Implementing physical exercise training to enhance strength, resistance, coordination, and stabilization might be beneficial in the field of interventional radiology to prevent WRMSDs.
Work-related musculoskeletal disorders in interventional radiology are a significant concern that cannot be ignored. These disorders not only affect the well-being and productivity of radiologists but also have a broader impact on the healthcare field.
It is imperative for healthcare institutions to implement ergonomic interventions and regular health check-ups to mitigate these risks. By prioritizing the health of our radiologists, we can ensure they continue to provide the highest level of care to their patients.
For more information about this topic, we invite you to visit our division for medical imaging technology and equipment ERI, and its resources for ergonomics and sonography.