Biopsies are an essential component of a physician’s cancer care toolkit. In a nephrologist’s toolkit, renal biopsies are equally important. Renal biopsy has experienced several modifications since its inception decades ago, including the recent incorporation of needle guides.
From the introduction of the Vim-Silverman needle in the 1950s to the development of the spring-loaded automated biopsy gun, clinicians have continually modified their methods to improve patient outcomes. The use of ultrasound guidance during these procedures has become widespread in the last two decades and has given practitioners the ability to carry them out with greater ease.
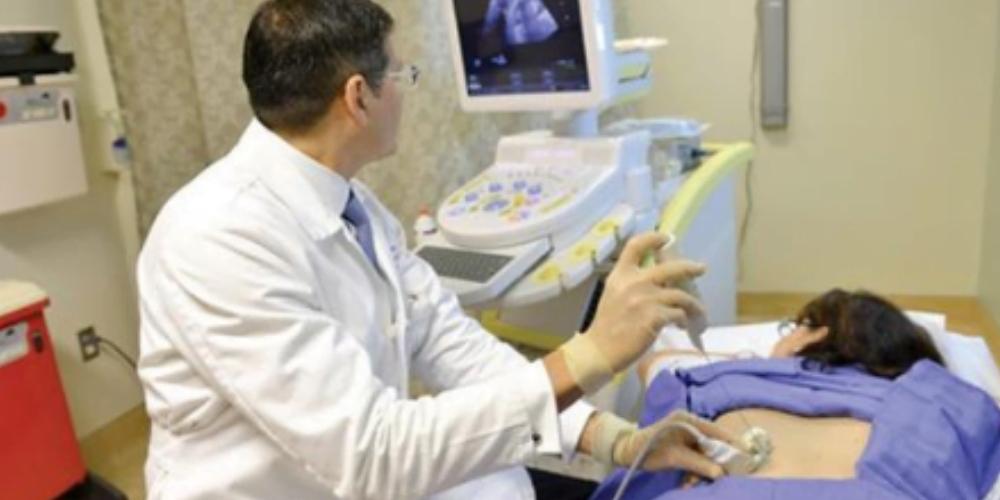
Currently, the majority of renal biopsies are conducted as ultrasound-guided procedures. At times, practitioners may opt to use computed tomography (CT) guidance; however, this comprises only a small portion of cases. The use of ultrasound is a significant contribution to the reduction of complication rates of renal biopsies. By providing a high-quality image, the nephrologist is able to clearly locate and extract samples from the target area.
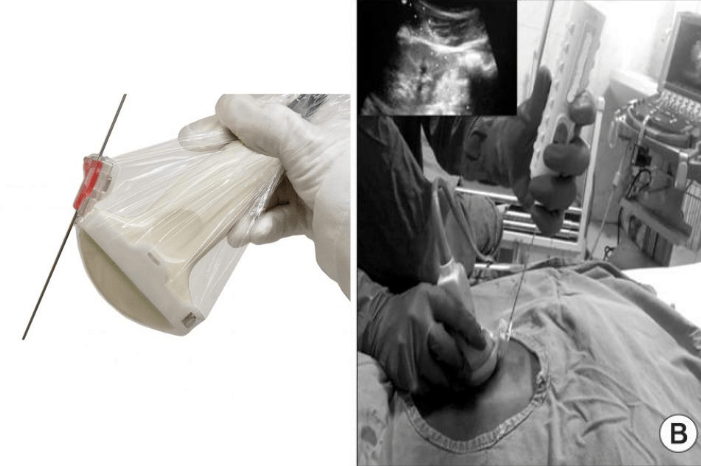
In recent years, nephrologists have also begun to use needle guides in their procedures. The guide works by holding the needle in a predetermined track and subsequently reduces the risk of path deviation. Clinicians have hypothesized that this reduction in path deviation signifies better outcomes, since it prevents the needle from hitting outside of the target area. Needle guides are commonly used in prostate and breast biopsies, but few studies had analyzed its efficacy in ultrasound-guided renal biopsies.
In a study published in 2018, researchers sought to determine whether needle guides had an impact on the safety of ultrasound-guided renal biopsies. They compared their findings to those of two previous studies — both of which had conflicting results. One of the studies found that needle guides improved patient safety during the procedure while the other did not identify a difference in outcomes.
Researchers conducted a retrospective single center study which compared biopsy yield, adequacy, and complication rates before and after needle guide use. In addition, the authors took into account clinical characteristics, type of investigation, indications, tissue yield, procedure adequacy, and rates of major and minor complications. The research team also considered the number of operators performing the procedure. This is a factor which they believe is “under-studied” but that may have a potential effect on procedure outcomes.
The study involved 343 biopsies performed over a 45 month period. Of these biopsies, 140 were performed without the use of a needle guide and 203 with a needle guide. There were no significant differences between patient groups in regards to baseline parameters, except that a higher number of diabetic biopsies were performed in the first period.
The overall rate of complications in the study was 1.7%. Five cases required angiography and two cases required a blood transfusion. In addition, the rate of minor complications was 8.4%. In the end, the authors found that the use of a needle guide in the procedure reduced the risk of complications by about one-third.

“Our study showed similar yields of glomeruli, improved biopsy adequacy as well as better safety, similar major complications, with significantly lower minor complication rates after the use of needle guides, even when the biopsies were performed by a single operator in the needle guide use period,” wrote the authors.
The main strength of the study was in the number of participants with advanced renal failure requiring hemodialysis, noted the authors.
The findings of the study signify that needle guides can play a role in increasing patient safety, especially as it relates to bleeding complications, which are some of the most common for renal biopsies. Depending on the site of hemorrhage, patients can experience bleeding complications in the form of perinephric hematomas, arteriovenous fistulas, and aneurysms. Complications such as these can present themselves as an asymptomatic drop in hemoglobin, bladder clots, and hematuria, as local pain, and as obstructive symptoms when the bleeding occurs in the pelvicalyceal system.
As a result of bleeding complications, physicians may need to perform subsequent invasive procedures. These include angiography, blood transfusion, cystoscopy, or surgery. This not only decreases patient comfort, but also results in higher costs. Today, however, only a minority of complications require invasive procedures and constitute 0.3% to 6.6% of cases. Thanks to the low risk of ultrasound-guided renal biopsies, a large number of healthcare facilities have begun performing them as day procedures in recent years. Nonetheless, physicians should still take into account that some patients may be at higher risk of complications than others, such as older individuals, females, and those with poor renal function.
The researchers concluded that transitioning to needle guides is generally safe and successful. According to their study, procedures which used needle guides saw significantly lower minor complications. Overall, needle guides provide a way for practitioners to increase the accuracy and precision of their ultrasound-guided biopsies.
General purpose (or surface) needle guides come in multiple configurations which allow them to be used for a variety of procedures, including biopsies, fine needle aspirations, nerve blocks, joint injections, and more. GP needle guides are also designed to fit a wide range of ultrasound transducers making them easy to integrate with your current equipment. These needle guides will hold the needle in place in the ultrasound plane for in-plane approaches, or perpendicular for out-of-plane procedures. In addition, they are helpful for reducing procedure time significantly. Being single-use makes these guides safe for patients and eliminates the need for time-consuming disinfection. Needle guides are also available for endocavity procedures.